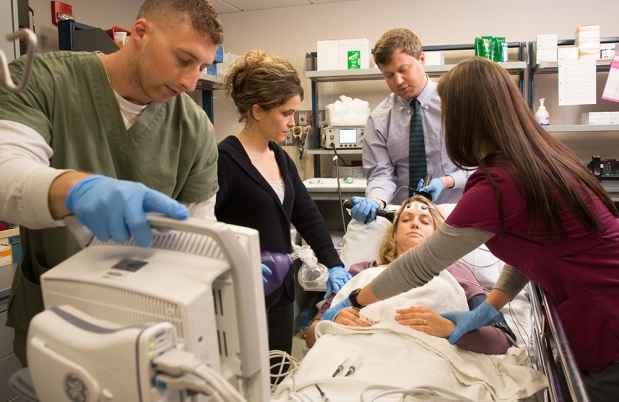
Electroconvulsive Therapy (ECT) Service
Helping individuals fight depression. Call us today to find out if ECT is right for you.
McLean’s Electroconvulsive Therapy (ECT) Service is dedicated to improving the quality of life for individuals with a broad range of mental health conditions. ECT is a highly effective conventional intervention for chronic depression, mania, catatonia, and schizophrenia.
McLean’s ECT treatment is best suited to adults who:
- Have severe or treatment-resistant depression, or other mental health conditions such as mania, catatonia, and schizophrenia
- Seek relief from their symptoms after trying treatment options that have not been effective
With components in clinical care, research, and education, McLean Hospital is a leading specialty center for electroconvulsive therapy, having conducted ECT treatments for over 60 years. Using a collaborative team approach, we aim to maximize the effectiveness of other treatments offered at McLean using emerging techniques and technologies.
Our dedicated and compassionate staff are dedicated to helping patients find the care they need.
Treatment Approach
Patients may have an entire series of treatments either on an inpatient or outpatient basis. The outpatient service allows patients to be treated and on their way home within two and a half hours.
Most patients who come to McLean to receive ECT will have 8-15 treatments over a period of three to four weeks. If you have excellent results, it is possible to transition to continued or maintenance ECT, if indicated. Your psychiatrist will work with you to decide how many treatments are needed.
After years of providing treatment and listening to feedback from patients, our program’s staff can ensure that your ECT treatment will be as comfortable as possible. Our staffing model allows patients to have their own nurses throughout the treatment and recovery period.
From how to know whether ECT is right for you to what to wear to your appointment, this helpful guide provides detailed information for patients and their families about electroconvulsive therapy treatment.
Learn more about McLean’s unique approach to depression treatment.
In Her Own Words
As a participant in McLean’s Deconstructing Stigma campaign, Cynthia shares her story of mental illness and her experiences receiving ECT treatments at McLean.

About ECT
Although ECT was introduced in the 1930s, its therapeutic use today is very different from what is portrayed as “shock treatment” in books and films. ECT is a relatively safe and effective procedure, providing relief from serious psychiatric symptoms much sooner than other therapies, such as medication and psychotherapy.
ECT is reserved for patients who have not responded to medication, who are having excessive side effects from medication or who are severely suicidal. Statistically, approximately 80% of patients treated with ECT respond well and get relief from their symptoms. An initial consultation with one of McLean Hospital’s ECT psychiatrists offers the opportunity to get information about ECT.
During electroconvulsive therapy, a patient is anesthetized and a small amount of electrical current is used to stimulate the brain. This produces a modified seizure, which, in turn, changes the activity of the brain. Some of these changes are similar to those seen with certain antidepressant medications in the way they relieve symptoms. The medications used for anesthesia prevent injury and patients feel no discomfort during the procedure.
“I was someone who was deathly afraid of ECT, but you and your wonderful staff helped me to overcome my fears. The treatments clearly helped me and it is so wonderful to be able to laugh, smile and enjoy my life again.”
– A patient at McLean’s ECT Service
Like any medical procedure, ECT does pose some risk. To minimize the risk, every patient has a medical clearance, including a physical examination, blood tests and an electrocardiogram (EKG) before beginning ECT. The physical examination is performed at McLean by a clinician from the Internal Medicine and Primary Care Clinic.
ECT has some possible side effects, such as headache, muscle pain, memory problems, and, rarely, nausea and vomiting. Most people who have treatments report very few side effects.
The great majority of patients will have only minor problems with memory, though some will experience no difficulties at all. While these problems usually subside, there is no way to predict their extent. The psychiatrist will discuss this potential side effect in greater detail during consultation.
Learn More About ECT
What Is Electroconvulsive Therapy?
Admission & Cost
Admission
ECT is a highly effective conventional intervention and is ideal for individuals struggling with chronic depression, mania, catatonia, and schizophrenia. ECT treatment can also be effective for those who have not met with success with other types of care.
For further information about our program or to refer a patient, please call:
Phone: 617.855.2355 (press 2 to speak to an ECT nurse during business hours)
Referral Form
Referring clinicians should fill out the form below so that we may determine whether the program is good fit for the individual and gather the appropriate patient information.
Cost
McLean accepts Medicare, Massachusetts Medicaid, and many private insurance and managed care plans.
More information on insurance providers accepted by McLean Hospital may be found on the Mass General Brigham website. You may also find it beneficial to review McLean’s patient billing and financial assistance information.
Treatment Team
Program Leadership

Paula Bolton, MS, CNP, ANP-BC, Program Director
A nurse practitioner in the Internal Medicine Department at McLean Hospital for more than 25 years, Ms. Bolton has focused on health promotion and disease prevention for psychiatric patients. She was instrumental in both the expansion of the inpatient and outpatient Electroconvulsive Therapy (ECT) Service and the development of the Transcranial Magnetic Stimulation (TMS) and Ketamine Services on the Belmont and Middleborough campuses.

Stephen J. Seiner, MD, Medical Director
Dr. Seiner serves as director of McLean’s Psychiatric Neurotherapeutics Program, which includes ketamine, electroconvulsive therapy, and transcranial magnetic stimulation. He is also an assistant professor of psychiatry at Harvard Medical School. Dr. Seiner has published book chapters and journal articles, and has lectured in multiple venues.

John B. Roseman, MD, Associate Director
Dr. Roseman has interests spanning a broad range, with expertise in bioinformatics, medical education, and neurotherapeutics, particularly ECT. As the associate director of the ECT Service, Dr. Roseman shares oversight of the busiest ECT service in the country (more than 10,000 ECT treatments per year). He is also the McLean psychiatry clerkship director for Harvard Medical School, helping train medical students at McLean.
Staff and Associates
A highly qualified staff of psychiatrists and registered nurses, along with anesthesia experts from the Massachusetts General Hospital, have extensive experience in administering ECT and in caring for patients who undergo the procedure for such treatment-resistant conditions as depression, mania, catatonia, and some psychotic illnesses.
Frequently Asked Questions
Where is the ECT Service located?
The program is located on the Belmont campus, in the de Marneffe Building. For more information on directions, parking, and local accommodations, please visit our Maps & Directions page.
Who benefits most from ECT?
ECT is an outpatient service that focuses on treating individuals struggling with depression or other mental illness who are not responding to medications and psychotherapy.
In addition, those who are experiencing severe symptoms of depression or other mental illness that are threatening their health or safety may be good candidates for ECT, which can often work more quickly than medication.
What happens at a ECT appointment?
Most patients have questions about what to expect at their appointment. Read more about how to prepare for ECT and what happens during a treatment session in our Guide to ECT Treatment at McLean found below.
Is family involved in treatment?
Family can be involved in the consultation for ECT and are welcome in the ECT suite. Family members are invited to join meetings with the doctor after each treatment to review the treatment plan.
Is smoking permitted?
Smoking is allowed in designated outdoor areas only. No smoking is allowed inside any of our buildings.
Are cell phones and other electronics allowed?
Cell phones are allowed in the ECT suite, but cell signal is poor. There is a cordless phone in the recovery room or staff can place a call.
Additionally we are just below the cafeteria—which does get a better signal—and family members who want to wait there can take a pager from the ECT suite and will be paged when the treatment is complete.
Can former patients access their medical records?
All requests for medical records should be directed to McLean’s Health Information Management Department.
Are support groups offered?
To complement our programs’ services and encourage individuals’ initiatives in their own treatment course, many self-help groups are hosted by McLean.
There is a monthly ECT support group meeting at McLean, which patients, family members, and/or those contemplating ECT are welcome to attend.
More information on patient and family resources is located below.
Guide to ECT Treatment at McLean Hospital
Electroconvulsive therapy (ECT) is used to treat a variety of psychiatric conditions, including depression, mania, catatonia, and some psychotic illnesses. During the procedure, a mild electrical current is delivered to the brain, which produces a modified seizure. ECT is a safe procedure that causes no pain or discomfort for patients.
The Electroconvulsive Therapy Service is located on McLean’s Belmont campus in the de Marneffe Building, Ground Floor. For more information call 617.855.2356.
ECT has been clinically proven to work. A vast majority of patients show measurable improvement and many report that they feel “like themselves” again after treatment. Experts believe that the improvements may be caused by the seizure changing the amount of certain chemicals in the brain.
ECT is often preferable for patients who don’t respond well to medications, have excessive side effects from medications, or are actively suicidal. Your clinician will help you decide whether or not ECT might be appropriate and beneficial for you and your symptoms.
Patients are welcome to schedule a visit to the ECT suite before beginning treatment. This helps some people feel more comfortable/less anxious about the procedure.
ECT staff includes psychiatrists specially trained in ECT; anesthesiologists from Massachusetts General Hospital; advance practice nurses specially trained in ECT; registered nurses with special training in ECT and post-anesthesia care; mental health specialists who work with the nurses to provide care; and physicians from the Internal Medicine Department who are on call at all times.
Risks and Side Effects
Before undergoing the procedure, medical clearance is necessary to make sure there are no medical conditions that might interfere with ECT treatment.
Some patients may experience changes in heart rate or blood pressure during the procedure, but these changes are usually short-lived and easily treated with medication. More serious problems are rare, but our staff is always prepared to give appropriate medical care as needed.
Memory loss is the most common side effect of ECT. Patients may experience some mild short-term memory loss and forgetfulness during the treatment. This side effect, however, usually ends shortly after the treatment course has ended.
Less frequently, patients have lingering memory loss of some events in the weeks to months before treatment. The memory loss is usually not significant, but we work hard to limit this side effect.
Other possible side effects are headache, muscle aches, nausea, and vomiting. Most people who have ECT treatment report very few side effects, and most are minor and easily treated.
Preparing for Treatment
ECT can be administered to patients who are in the hospital, living at home, or in a community setting (e.g., nursing home or group home). McLean Hospital has a dedicated ECT Suite located in the de Marneffe Building.
Most patients will have an initial course of 8-15 treatments, which are administered 3 times per week, on Mondays, Wednesdays, and Fridays.
This 3-4 week course of initial treatment is usually followed by a taper phase and maintenance treatments may continue—weekly or less frequently—to prevent relapse. Tuesdays and Thursdays are reserved for maintenance treatments.

ECT is a safe procedure that causes no pain or discomfort for patients
To prepare for your appointment, you cannot eat or drink anything after midnight on the day of your treatment. This includes water, gum, mints, cough drops, and most medications. If you forget and have something to eat or drink, you MUST tell the staff on your unit or the ECT staff. You also should not smoke the day before or the morning of treatment.
Before coming in for treatment, please dress in comfortable clothing, including a short sleeve shirt or a shirt that can be rolled up easily to check blood pressure and start intravenous (IV) treatment. Do not wear perfume, other scented products, makeup, or nail polish. If you have dentures, contact lenses, or nose, lip, or tongue piercings, they must be removed before treatment.
Please bring an updated list of all your medications to each treatment.
At Your Appointment
Once you arrive at the clinic, let the secretary know you are here. You will remain in the waiting area until an ECT nurse brings you to the treatment area.
While in the treatment area, you will be asked to complete some questionnaires on the computer and do a memory assessment with a nurse. The nurse will also ask about your mood and how you’re feeling physically.
If you are an outpatient, the ECT staff will check your weight, temperature, blood pressure, and pulse and make sure that you haven’t had anything to eat or drink. These things will be checked for inpatients while they’re still on the unit, before staff brings them to the ECT clinic.
At your first treatment, the anesthesiologist will review the medical information in the chart and ask some questions before treatment begins.
A nurse will then put medical monitoring equipment on you just before treatment starts. This equipment will measure your blood pressure, oxygen levels, and heart rate throughout the treatment. Next, an intravenous (IV) catheter for delivering anesthesia will be placed in your arm or hand. To ensure minimal discomfort, a very small catheter is used.

McLean is a leading specialty center for ECT
Anesthesia will be delivered through this catheter. You will fall asleep in less than one minute and will remain anesthetized for 5 to 10 minutes. After you are asleep, you will be given a medication that relaxes your muscles. This reduces body movement when you have the seizure produced by ECT.
During Treatment
You will be in the treatment room for approximately 10 to15 minutes. You will not feel any pain or discomfort during treatment.
While you are asleep under anesthesia, the ECT clinician will begin by placing two small stimulating electrodes on your forehead, which will record your brain waves during treatment.
While the ECT clinician is delivering mild electrical current to your brain, the anesthesiologist will help you breathe by giving you oxygen through a ventilation mask. During this time you will be under continuous monitoring.
After the treatment is over, you will be moved into the recovery room. Most patients will wake up a few minutes after they’ve arrived in the recovery room.
Recovery Room
Your nurse will stay with you throughout your recovery and will continue to check your blood pressure, pulse, breathing, and oxygen level. A plastic oxygen mask will be placed over your nose and mouth to give you additional oxygen until you are wide-awake. When you first wake up, you might be slightly confused. This is a normal reaction to treatment.
After about 30 minutes, you will be ready for something to drink. Soon afterward, if you are staying in the hospital, staff from your unit will pick you up and bring you back to the unit in a wheelchair. This is just a safety precaution.
After spending 45 minutes in the recovery room, outpatients will need to spend the next hour and 15 minutes in the recovery lounge. (Most patients are ready to leave two hours after treatment.) Just before it is time for you to leave, a nurse will check your temperature, blood pressure, and pulse.
A clinician will also evaluate you at this time. Finally, you will be given discharge instructions and an appointment for your next treatment.
After Treatment
Soon after treatment, most people are ready for something to eat. Inpatients can have a meal when they return to their units, and outpatients can have a light meal in the recovery lounge.
Some patients feel sleepy after treatment and will want to take a nap, and others are wide awake and ready to resume their usual activities. Whatever you choose to do, it’s important that a responsible adult be with you for the rest of the day.
“Dr. Stephen Seiner, along with the entire ECT staff (from the secretary to every nurse), have been available to answer any questions and have done everything they can to put both my husband and me at ease.”
– A McLean ECT patient
You should not exercise vigorously, drive a car, operate machinery, or drink alcohol for the rest of the day. You should take your daily medications, and if you have muscle soreness or a headache, over-the-counter pain relief medication should help.
Most patients will notice a positive change in their mood after they have had five or six treatments. Certain behavioral changes, however, may occur before you start feeling better mentally. If you were not able to sleep or eat, you may begin to sleep better and have an increase in appetite.
If you were sleeping too much and had no interest in activities, you might start getting out of bed more and wanting to get involved with friends and family. Family members and/or staff usually notice improvement in a patient’s mood before the patient does. Very soon afterward, the patients themselves report that they’re feeling better.
Patient & Family Support
Individuals who are taking part in ECT have many questions and concerns. Our goal is to provide the resources and support necessary to make a comfortable and informed choice to proceed with ECT. Because of the many fears and misconceptions surrounding the treatment, comprehensive support is essential.
Psychiatrists, nurses, and organized support groups at McLean and other institutions often work together to answer questions, alleviate concerns, and help keep treatment and recovery on track.
What many people don’t know, however, is that support is also available to help families and caregivers of ECT patients. This support is equally important, because family members and caregivers play a crucial role in helping their loved ones consider the treatment, engage with the therapy team, and move toward recovery.
Because of the many concerns patients and families have about ECT, we’ve created patient and family support groups. Right now, McLean offers a monthly support group for outpatients, education groups on our inpatient units, and a group focused on improving memory and cognition after ECT is completed.
Family involvement is central to the success of patient recovery, and it is an important aspect in each one of our groups.
Our ECT support groups offer a safe place where all aspects of the treatment can be discussed openly. Patients and their family members can draw on the experiences of other patients who attend the group. Often, former patients will attend groups to share their experience and tell attendees how much ECT has helped them get back to their life.
The groups provide an opportunity to assure patients and families that modern ECT techniques use anesthesia and muscle relaxants to maximize safety and minimize side effects.
Patients and caregivers can also hear firsthand accounts of how memory impairment is experienced by other patients having ECT. The support groups give us the opportunity to separate myth from fact and work toward dispelling stigma.
Another important aspect of ECT family support is that it encourages people to take care of themselves while they are taking care of their loved ones. Helping a family member with severe depression is an important, but stressful, full-time job.
In talking to families at McLean, we often hear about “caregiver fatigue.” Through our groups, we help caregivers optimize all of the support systems available to them inside and outside the hospital. We let them know that there’s a whole team of people who are here to help and support them through the ECT process.
McLean is here to help. Call us today at 617.855.2355 to talk to our team about whether ECT is the right option for you, a loved one, or a patient.